What's New
24 June, 2020
The North Shore Patient: one man’s experience
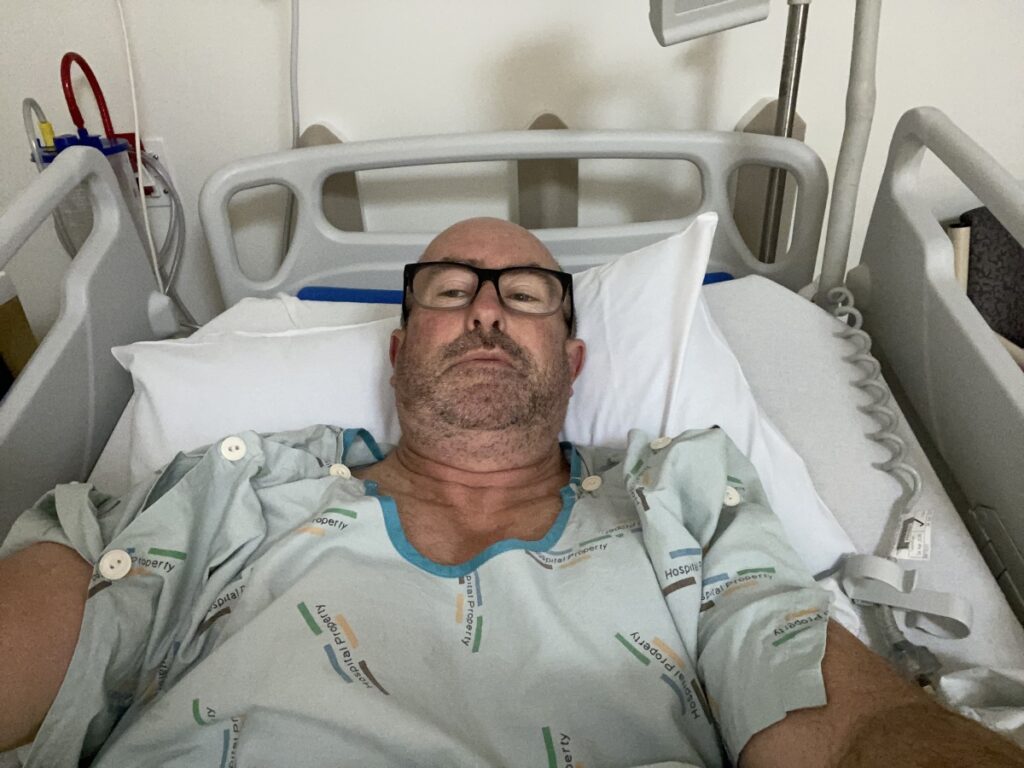
My nurse Sue was using a nifty system of short, sheer plastic tubes to help slip on compression socks. I couldn’t put the socks on myself as my pain was so intense. It was five o’clock on a Sunday afternoon and I was being prepared for emergency surgery on an abscess – cause unknown – but common in New Zealand at the moment apparently.
My weekend was meant to have taken a different course. I should have been in the stand at Eden Park cheering the Blues.
But my unreliable body had different ideas. I was in the Short Stay Ward at North Shore Hospital, along with many others who would have also rather have been somewhere else.
The road to surgery began the previous Thursday. I’d played squash the night before (losing in the regular Devonport-Belmont club challenge), had nothing to drink, but woke with what felt like a crashing hangover. Over the next couple of days I felt cold and listless and started going to bed early. By Saturday the tiredness had become chronic and I’d developed pain in the upper groin.
After my first interclub tennis match of the winter season that day, movement was becoming difficult, exhaustion gathering pace. From the neighbouring court, former NZ number one Mark Nielsen paused in his coaching to observe: “You’re not doing much work to help your partner, Rob.”
Yep, the unreliable body wasn’t playing ball. Next day, it was worse. Trying to get up the motiviation to head into work for a couple of hours, I was instead glued to the couch. With a trip to the Blues looking unlikely, my partner Jo decided a trip to Shorecare was needed.
By the time I got there, I was seriously crook. My temperature was closing in on 39, signing the admission forms was a major effort and I was getting muddled: I gave my two previous trips to hospital as happening in 1918 and 1919 instead of 2018 and 2019.
I’d already google-diagnosed my condition as haemorrhoids, which I’d had once before. Wrong. Doctor Andy immediately suspected an abscess: treatment needed immediately.
After a couple of calls, he got through to the North Shore Hospital general-surgery doctor on duty. Forms were sent over and I was booked in without having to sit for hours in the Emergency Department. I only had to collect my Robert Michael Drent wrist band at the desk. I was amazed at the efficiency.
It was the first of many ticks I would give New Zealand’s health service over the next few days. Hiccups did occur. Jo ran into a nurse friend on the ferry to the Blues match who said:
“He’s most likely got a blocked duct – they’ll fit him at the end of the day after all the more important operations.”
In fact, my operation was bumped. Two emergency cases came in. I left nurse Sue’s socks on hoping to get a lucky break first thing the next day.
I seem to have a personality that can endure airline terminals, long flights and hospital wards. The feeling of entrapment and interminable waiting that drives many people nuts has never bothered me too much. In fact, I find the opposite: there’s always heaps going on. Humans in transit – at airports to foreign countries, in hospitals to destinations unknown – creates a tension. No one can really predict what their outcome will be.
My ward-mate that Sunday was a woman in her 70s who had been transported by wheelchair from a nearby rest home. She had had bowel problems for days, but they had worsened.
Medical institutions and ethics committees stress and fuss over the intricacies of patient privacy and confidentiality, but the irony is that once you reach a medical ward there is no privacy at all. After a couple hours lying less than a metre away from your neighbour, you often know almost everything about them, including often-lengthy medical histories and their drug-taking regimen, all broadcast through a curtain of supposed separation.
My ward mate was plagued with numerous conditions and tired of a body more unreliable than mine. But she had a sense of humour: “I tell you what,” she said to a friend on the phone, “if I knew it was going to be like this in my 70s, I’d have had more fun in my 50s.”
She had a full life too. A list of dinners, lunches, appointments and catch-ups with mates needed to be cancelled. She called nextdoor neighbours and asked them to water her new plants: “Just a little drink – I know you can be a little heavy-handed.”
Doctors were working on a plan for her, but her pain got worse as the evening wore on. Before midnight, a throng of medical staff were next door pushing and prodding, asking more questions. Had a scan revealed new information?
“Don’t worry my darling we’re taking care of you,” a nurse with a northern-English accent said. As she was moved to another ward for more critical care, I silently wished her well.
Day Two: Mornings can start early in hospital. Just after midnight, it was announced I would be moved to Cullen – a elective surgical ward – at 2 am, in the hope I would be prepped and ready to be first up the next day.
Since my arrival, I’d been gingerly asking hospital staff what their feelings were about Covid-19. From the main entry, through the emergency department, to the corridors and wards, there was a we’ve-dodged-a-bullet kind of euphoria. If Covid had taken hold, “We wouldn’t have coped,” said one nurse. New Zealand simply didn’t have enough beds or ventilators. Hospital staff were also relieved PPE equipment didn’t have to be put to the test. “There is no way it can protect you completely,” she said. Another staffer: “We’re really happy to see the patients back.”
A hospital devoid of most of its patients must have been a strange place indeed.
The Cullen Ward was set up as a Covid-19 receptacle ready to take the expected influx of cases. It didn’t host any. The only case at North Shore Hospital was housed in the infectious-diseases ward.
Cullen is eight years old, I’m told, which surprises me: it appears brand-new. Perhaps it is the pre-Covid cleaning.
But then the whole hospital is spick and span. I’ve been a patient half a dozen times over the last couple of years (heart issues), and while the hospital was never dirty, the level of cleanliness last week was next-level. Wards and rooms were regularly cleaned when I was there, and it wasn’t a quick sweep or dust either.
I watched one cleaner meticulously wipe down doors, door knobs, a wall clock, along tops of picture frames and window sills. It appeared to be systematic. “Cleanliness and hygiene are top priorities,” a new graduate nurse told me almost mantra-like.
It was reassuring as I moved towards the uncertainty of the surgical ward. Suddenly, just after 7.30am, nurse Kara arrived: “We’ve got to get you ready.”
“If Covid had taken hold, “We wouldn’t have coped,” said one nurse. New Zealand simply didn’t have enough beds or ventilators. Hospital staff were also relieved PPE equipment didn’t have to be put to the test.”
More blood tests, temperature checks, blood pressure and then we’re off. No orderly comes quickly, so Kara decides she can drive the bed. She’s joined by a charge nurse, and as we spin towards the pre-op room a hospital support worker mocks her cornering technique.
It struck me as a happy workplace. Jokes and banter are missing on miserable job sites.
In pre-op, the unreliable status of my body was confirmed by the anaesthetist and surgeon, with my heart history (underlying heart condition, plus stent and atrial fibrillation operations) described as “complicated” and “difficult”.
The anaesthetist asked me about exercise. I was back tramping, playing tennis and squash, I replied. He was also a squash player – who seemed to have B grade aspirations. I found this strangely comforting as we filled in the usual consent forms informing of the risk of death on the operating table.
“Genetic predisposition” was the likely cause of my abscess, the surgeon said. Unreliable body conspiring against me again, I thought.
The operation went smoothly, and an hour later I was back in Cullen sleeping off the anaesthetic alongside a dose of daytime TV. I never knew Suzanne Paul was back on screen (Thin Lizzy Puffer Eye Remover – seven minutes a day removes 15 years), and I must watch more of Al Jazeera’s news coverage. I was kept in overnight to have doses of antibiotics intravenously.
I was ready to head home first thing next day, but there was a complication: swollen testicles. My doctor says this needs a scan. North Shore Hospital gets another tick for thoroughness.
On the way to the radiology room, the orderly says he’s only been in the job eight weeks. Between jobs when lockdown hit, he took the role as a safe employment option with uncertain months ahead. “It’s been a great job, though, with great people and I like meeting the patients.” He was also happy his belt had crept in a couple of notches from the 10,000 plus steps he was doing on the wards every day.
In radiology, a well-dressed woman is in for deep vein thrombosis testing. Her phone goes off and its her son wanting money transferred over for some takeaways. “Kids sucking us dry even when we’re in hospital,” she says. “Cell phones are the problem,” I say.
I’m tested by an experienced operator and a trainee, who are using a new machine. Numerous times during my visit an experienced health professional showed a more recent graduate correct techniques during my treatment. Student nurses were common: expertise was being passed on, institutional knowledge was being built. The system was working.
The scan revealed nothing exceptional and almost on cue, my mate Dr Doom (a friend known for fatalistic view on life) arrived to offer a lift home. My brief test of the health system was concluded.
Except it wasn’t. Once home the abscess plug fell out and I was back at the emergency department, being readmitted.
There, I turned to find a policeman at my shoulder, in charge of a man slumped in a chair. It was “Bob”, sometimes known as “walkie talkie man”, who has spent the last couple of decades walking up and down Lake Rd, often sleeping rough on Maungauika.
The abrasions to his face and hands were suffered in a fall on Lake Rd, the policeman said. Form filling was difficult, as he was “homeless”. Later, I thought I should have said Devonport was his home. I know locals have helped him out of a few scrapes over the years, and here was an obvious extension: wider community care for the most vulnerable.
A massive review of District Health Boards was announced during my second stay. But from my patient-centric view, many things at North Shore Hospital are working just fine.
On the way home my taxidriver, originally from Pakistan, has lived in New Zealand since 1993. Without tourists, taxi drivers are doing it hard, but he’s with Co-op and is fortunate the company has contracts with the three district health boards to take people for dialysis, ACC appointments and the like.
“We are so lucky to live here – in Pakistan people are dying everywhere (from Covid-19),” he said. After a difficult few months running a newspaper business through Covid-19 – only made survivable by the government wage subsidy – and my brief trip through the health system, I agreed. “Yes we are very lucky,” I said.
The Rangitoto Observer can be downloaded online here.

Please consider supporting The Rangitoto Observer by clicking here:

